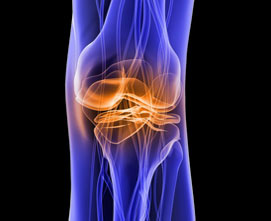
Biological strategies for restoring articular cartilage
Degenerative joint diseases, particularly osteoarthritis, are among the leading causes of chronic pain and disability worldwide. The primary structural feature of these conditions is the gradual degradation of hyaline cartilage, accompanied by subchondral bone remodeling, synovial inflammation, and altered joint biomechanics. In advanced stages, significant cartilage loss results in severe pain, stiffness, and functional limitation, often necessitating joint replacement surgery.
Contemporary orthopedics and regenerative medicine focus on strategies that may slow or partially reverse degenerative changes without resorting to prosthetic implantation. Central to these approaches is the stimulation of cartilage repair and the creation of an intra-articular environment conducive to tissue regeneration.
Articular cartilage has limited intrinsic regenerative capacity. It is avascular, contains relatively few chondrocytes, and exhibits low metabolic activity. As a result, spontaneous repair of cartilage defects is often incomplete and structurally inferior. Therapeutic interventions therefore aim to activate residual cellular potential and modify biological pathways involved in tissue maintenance.
One biological approach involves the use of platelet-rich plasma. Platelets release growth factors such as platelet-derived growth factor and transforming growth factor beta, which promote cell proliferation and extracellular matrix synthesis. Intra-articular injections of platelet-rich plasma may reduce inflammation and improve symptoms in early degenerative stages, although structural restoration remains variable.
Autologous chondrocyte implantation represents a more advanced regenerative technique. This procedure involves harvesting chondrocytes from the patient, expanding them in vitro, and reimplanting them into the cartilage defect. The goal is to generate tissue resembling native hyaline cartilage. This method is primarily indicated for focal cartilage lesions rather than diffuse advanced osteoarthritis.
Mesenchymal stem cells have attracted significant research interest. These multipotent cells can differentiate into chondrogenic lineages and secrete bioactive molecules that modulate inflammation and promote tissue repair. Intra-articular administration of mesenchymal stem cells has been associated with pain reduction and functional improvement in selected patients, although long-term structural outcomes are still under investigation.
Bone marrow stimulation techniques, including microfracture, aim to recruit progenitor cells from the subchondral bone into the cartilage defect. The resulting repair tissue is predominantly fibrocartilage, which has inferior mechanical properties compared to hyaline cartilage but may provide symptomatic relief and partial structural coverage.
Tissue engineering expands regenerative possibilities through the use of biomaterial scaffolds. Three-dimensional matrices serve as structural frameworks for cell attachment and tissue formation. When combined with autologous cells or growth factors, these scaffolds support more organized cartilage regeneration and enhance integration with surrounding tissue.
Disease stage plays a crucial role in therapeutic selection. Regenerative approaches demonstrate greater effectiveness in early or localized lesions where joint alignment and stability are preserved. In advanced osteoarthritis with substantial deformity and joint instability, biological interventions have limited capacity to restore function.
Biomechanical factors must also be addressed. Weight reduction, correction of malalignment, and targeted physiotherapy reduce mechanical overload on the joint and support regenerative processes. Without addressing mechanical stressors, biological treatments may have diminished efficacy.
Magnetic resonance imaging is an essential diagnostic tool in treatment planning. It allows evaluation of cartilage thickness, subchondral bone changes, and synovial inflammation. Imaging findings guide the selection of appropriate regenerative techniques and help monitor structural response over time.
Although joint replacement remains an effective solution for end-stage disease, early implementation of regenerative strategies may delay surgical intervention and preserve native joint structures. Continued research aims to optimize cell sources, scaffold materials, and growth factor combinations to enhance long-term outcomes.
In summary, cartilage regeneration without joint replacement represents a promising direction in modern orthopedics. Biological therapies, cell-based techniques, and tissue-engineering innovations target multiple aspects of the degenerative process. Ongoing clinical studies seek to refine indications, improve durability, and establish standardized treatment protocols.
Write a review
Required fields are marked with *
Categories
- News (42)
- Therapy (31)
- GP (23)
- Endocrinology (8)
- Cardiology (8)
- Ortopedics (4)
- Dermatology (3)
- urology (1)
- Check-up (1)
- Ultrasound (1)
Articles
Archive
- February 2026 (8)
- January 2026 (8)
- December 2025 (6)
- November 2025 (6)
- October 2025 (6)
- September 2025 (6)
- August 2025 (7)
- July 2025 (4)
- June 2025 (11)
- May 2025 (9)
Categories
- News (42)
- Therapy (31)
- GP (23)
- Endocrinology (8)
- Cardiology (8)
- Ortopedics (4)
- Dermatology (3)
- urology (1)
- Check-up (1)
- Ultrasound (1)





Comments (0)