
Clinical decision support through machine learning
The integration of artificial intelligence into healthcare represents a significant этап in the digital transformation of medicine. In clinical practice, artificial intelligence primarily refers to machine learning algorithms and deep neural networks capable of analyzing large volumes of structured and unstructured medical data. These systems are designed to support, rather than replace, physicians by identifying patterns and generating predictive insights that may not be immediately apparent through conventional analysis.
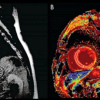
Medical imaging is one of the most advanced areas of application. Deep learning algorithms trained on large annotated datasets can detect radiographic abnormalities on X-rays, computed tomography scans, and magnetic resonance imaging studies. Such systems are capable of identifying pulmonary nodules, intracranial hemorrhage, ischemic lesions, fractures, and tumor-related changes with high sensitivity. Automated image analysis can reduce interpretation time and assist in prioritizing urgent cases.
In cardiology, artificial intelligence is applied to electrocardiogram interpretation and arrhythmia detection. Machine learning models analyze waveform patterns to identify subtle irregularities that may indicate atrial fibrillation, conduction disturbances, or early myocardial dysfunction. Predictive algorithms combining clinical and laboratory variables are also used to estimate cardiovascular risk and guide preventive strategies.
Oncology benefits from artificial intelligence in histopathological assessment. Digital pathology platforms enable automated evaluation of biopsy specimens, classification of tumor subtypes, and estimation of proliferation indices. By standardizing image interpretation, these systems may enhance diagnostic consistency and support personalized treatment planning.
In intensive care settings, predictive analytics play a critical role. Continuous monitoring data, including heart rate, blood pressure, oxygen saturation, and laboratory values, can be processed by machine learning algorithms to anticipate clinical deterioration. Early warning systems may predict sepsis, respiratory failure, or hemodynamic instability before overt symptoms develop, enabling timely intervention.
Electronic health records provide another domain for artificial intelligence implementation. Natural language processing techniques allow extraction of clinically relevant information from free-text documentation. Automated summarization tools can generate structured reports, reduce administrative burden, and improve accessibility of patient data.
The development of reliable artificial intelligence systems depends on high-quality training datasets. Large, diverse, and accurately labeled data are essential for building robust predictive models. Insufficient representation of certain demographic or clinical groups may result in reduced accuracy and unintended bias, underscoring the importance of careful dataset curation and external validation.
Algorithmic bias and transparency are central ethical considerations. Clinicians must understand the rationale behind algorithmic outputs to ensure safe integration into decision-making processes. Explainable artificial intelligence models are increasingly prioritized to provide interpretable insights rather than opaque predictions.
Regulatory oversight is evolving to address the unique challenges posed by adaptive algorithms. Validation in real-world clinical environments, ongoing performance monitoring, and clear delineation of responsibility are essential components of safe implementation. Integration into clinical workflows must be seamless and supportive rather than disruptive.
Despite technological advances, artificial intelligence remains an adjunct to clinical expertise. Diagnostic reasoning, contextual interpretation, and individualized patient care require human judgment. The most effective model is collaborative, in which algorithms enhance analytical capacity while physicians retain ultimate responsibility for clinical decisions.
In conclusion, artificial intelligence is reshaping disease diagnosis through advanced data analysis, imaging interpretation, and predictive modeling. As validation studies continue and ethical frameworks mature, these technologies are expected to become integral components of modern healthcare systems, improving accuracy, efficiency, and patient outcomes.
Write a review
Required fields are marked with *
Categories
- News (42)
- Therapy (31)
- GP (23)
- Endocrinology (8)
- Cardiology (8)
- Ortopedics (4)
- Dermatology (3)
- urology (1)
- Check-up (1)
- Ultrasound (1)
Articles
Archive
- February 2026 (8)
- January 2026 (8)
- December 2025 (6)
- November 2025 (6)
- October 2025 (6)
- September 2025 (6)
- August 2025 (7)
- July 2025 (4)
- June 2025 (11)
- May 2025 (9)
Categories
- News (42)
- Therapy (31)
- GP (23)
- Endocrinology (8)
- Cardiology (8)
- Ortopedics (4)
- Dermatology (3)
- urology (1)
- Check-up (1)
- Ultrasound (1)





Comments (0)