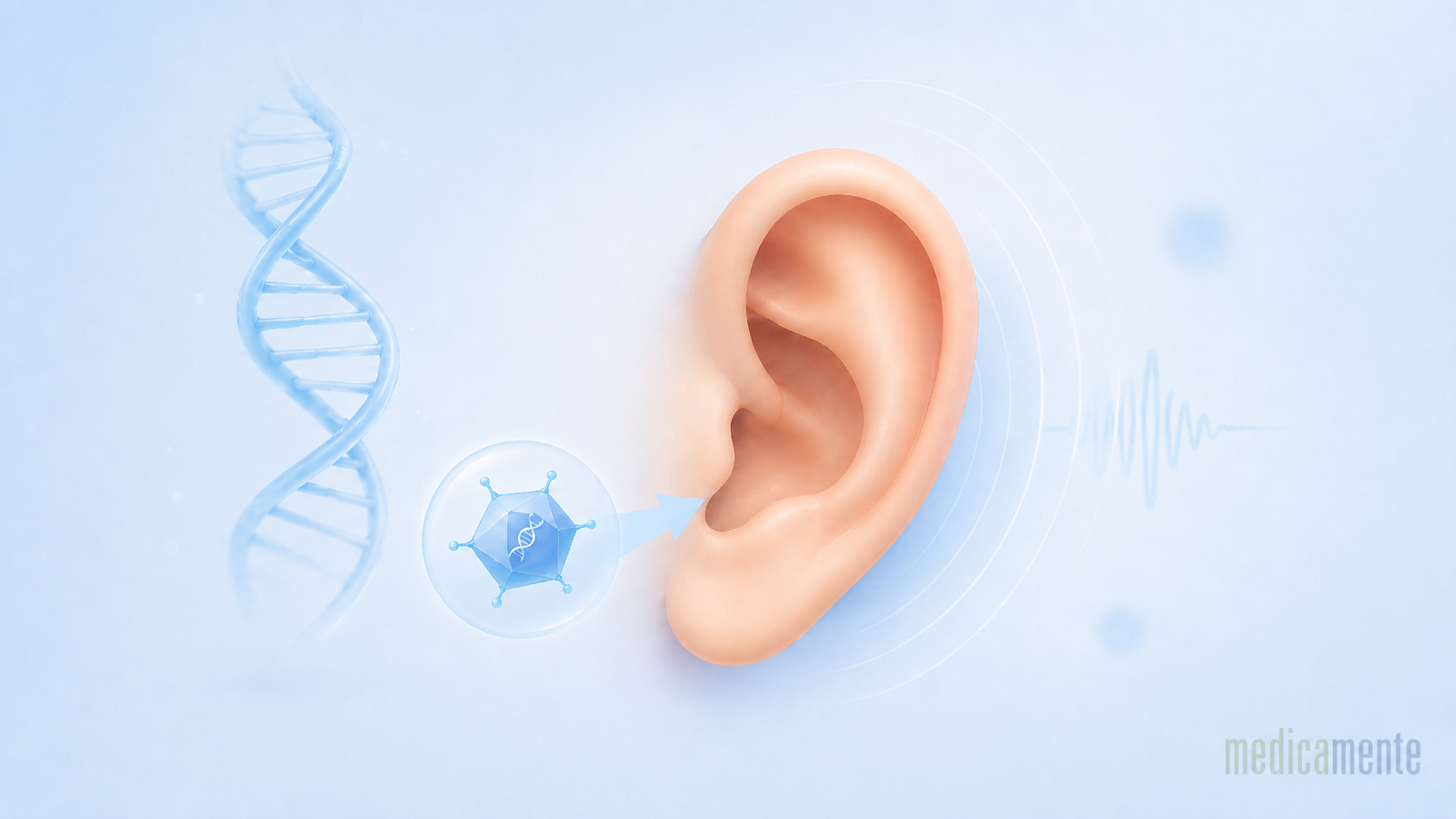
When medicine begins restoring hearing at the genetic level
Gene therapy for hereditary deafness has become one of the most illustrative developments in modern medicine because it demonstrates a shift from compensating for a defect to correcting it at the molecular level. For decades, severe congenital hearing loss was viewed mainly as a condition in which medicine could offer technical support, rehabilitation, communication training and, in selected cases, cochlear implantation. New approaches are changing the logic of treatment itself: the goal is not only to transmit sound signals around the damaged link, but also to restore the biological function disrupted by a specific genetic cause.
A particular focus has been therapy targeting mutations in the OTOF gene. This gene encodes otoferlin, a protein required for signal transmission from sensory cells of the inner ear to the auditory nerve. In patients with biallelic pathogenic OTOF variants, outer hair cells may retain the ability to respond to sound, while the connection between the inner ear and the nervous system is impaired. This is why this form of deafness became one of the first logical targets for gene therapy: if the sensory structure is partially preserved, introducing a functional copy of the gene may theoretically restore the missing link in signal transmission.
The principle of treatment is based on delivering a functional copy of the gene into cells of the inner ear using a viral vector. In this context, the vector acts as a transport system: it should not cause disease, but instead serves as a way to deliver genetic instructions to the site where they are needed. The procedure is performed locally, by introducing the therapy into the region of the cochlea. This approach is fundamentally different from systemic drug therapy because the intervention is directed at a specific anatomical and molecular problem. The outcome depends not only on the genetic construct itself, but also on the patient’s age, preservation of inner ear cells, the technique of administration and the accuracy of molecular diagnosis.
The clinical significance of this technology is linked to the fact that congenital deafness affects not only sound perception, but also speech development, cognitive load, social adaptation and the educational trajectory of the child. The earlier access to auditory stimuli is restored, the greater the likelihood of speech skill development during a period of high neuroplasticity. This makes such therapy especially important in pediatrics. It does not eliminate the need for audiological follow-up, rehabilitation and assessment of speech development, but it may change the patient’s starting point: instead of permanent compensation for a deficit, there may be a chance of partial or substantial restoration of the natural auditory pathway.
Initial clinical data show that the effect may not be immediate, but may develop gradually over several months. This corresponds to the biological nature of the intervention: after gene delivery, cells need time to synthesize the protein, restore signal transmission and allow the auditory system to adapt to new sensory information. Reports on treatment outcomes indicate that a significant proportion of study participants demonstrated hearing improvement during the first months of follow-up. Such data are important not only as confirmation of the efficacy of a specific product, but also as evidence supporting the viability of the broader concept of local gene correction for inner ear disorders.
However, gene therapy for hearing loss is not a universal treatment for all forms of deafness. Hereditary hearing loss is highly heterogeneous: it may be associated with dozens or hundreds of genes, different types of cellular damage, developmental abnormalities of ear structures or combined syndromes. A therapy designed for OTOF-associated deafness will not automatically work for other genetic causes. This highlights the central role of genetic testing. Without precise molecular diagnosis, it is impossible to determine whether a patient is suitable for a specific therapy, what prognosis is realistic and which alternative methods remain the main options.
Comparison between gene therapy and cochlear implantation requires caution. Cochlear implants remain a major technology that has helped many patients gain access to auditory information. Gene therapy should not be considered a simple replacement for implantation in all cases. Rather, it forms a new treatment category for a strictly defined group of patients who have preserved the necessary cellular structures and have a confirmed relevant mutation. In the future, these approaches may not compete, but coexist: the choice will depend on the cause of deafness, age, condition of the cochlea, previous treatment and expected benefit.
From a medical perspective, it is especially important that such methods require long-term follow-up. It is necessary to assess not only hearing thresholds after several months, but also the durability of the effect, long-term safety, impact on speech development, possible inflammatory reactions, immune response to the vector and rare late complications. For any gene therapy, the duration of the result is a key issue. A one-time intervention appears attractive, but long-term data will determine how much it changes the standard of care and how widely it can be applied in clinical practice.
The ethical dimension also remains significant. Treatment is often considered for young children who cannot yet make decisions for themselves. Parents and physicians must consider not only medical indicators, but also cultural, social and communication-related aspects of deafness. It is important to avoid the simplified idea that hearing loss is only a defect that must always be corrected at any cost. An appropriate medical approach requires informed decision-making, respect for the patient’s family, precise explanation of benefits and limitations, and avoidance of exaggerated expectations.
The scientific value of this direction extends beyond audiology. The success of local gene therapy in the inner ear shows that organs with complex anatomy and highly specialized function can become accessible targets for molecular treatment. This opens prospects for other hereditary hearing disorders, as well as for diseases in which precise delivery of therapeutic material to a limited anatomical area is required. At the same time, the development of such methods will depend on access to diagnostics, manufacturing capacity, regulatory control and the ability of healthcare systems to integrate high-technology treatments into real clinical practice.
The main meaning of this development is not that medicine has obtained an instant solution to deafness. Its significance is deeper: clinical medicine is moving increasingly toward causal treatment of diseases that were previously considered irreversible. Gene therapy for OTOF-associated deafness shows how fundamental genetics, microsurgery, viral vectors, audiology and pediatric rehabilitation can come together in a single therapeutic process. For patients, this may mean a new level of opportunity, and for medicine, it confirms that precise molecular diagnosis is becoming not an auxiliary step, but the foundation for choosing treatment.
Write a review
Required fields are marked with *
Categories
- Therapy (49)
- News (48)
- GP (23)
- Cardiology (9)
- Endocrinology (8)
- Ortopedics (4)
- Dermatology (3)
- urology (1)
- Check-up (1)
- Ultrasound (1)
Articles
Archive
- May 2026 (9)
- April 2026 (8)
- March 2026 (8)
- February 2026 (8)
- January 2026 (8)
- December 2025 (5)
- November 2025 (6)
- October 2025 (6)
- September 2025 (6)
- August 2025 (7)
Categories
- Therapy (49)
- News (48)
- GP (23)
- Cardiology (9)
- Endocrinology (8)
- Ortopedics (4)
- Dermatology (3)
- urology (1)
- Check-up (1)
- Ultrasound (1)





Comments (0)